Translate:
We Have Moved To Our New Location!!!
EN
Translate:
We Have Moved To Our New Location!!!
EN
Parents should start brushing their child's teeth as soon as they erupt into the mouth. Brushing should be done at least twice daily, but it is preferable to brush after every meal and before bed. When brushing use circular motions and make sure that the area where the teeth and the gums meet are brushed well. If the gums have not been brushed well it is not uncommon to see bleeding from the gums, this will go away after several days of brushing the gums well.
Parents should brush their child's teeth until age seven. After age seven parents should supervise their child's brushing.

Children's teeth have more space between them but if your child's front teeth are touching they should be flossed because brushing alone will not remove the bacteria that cause cavities from between the teeth. Once a child's baby molars (back teeth) erupt they almost always are close together and will need to be flossed. This usually occurs between two and three years of age. For a fun and easy way to floss your kids' teeth we recommend GumChucks. Please ask us for a demonstration at our office.

Before your child's first tooth erupts you should use a fluoride free training toothpaste to massage your childs gums. After your child's teeth first erupt, usually
the front teeth, you may start to use a smear layer of fluoride toothpaste to brush your child's teeth. Children should only use a smear layer of toothpaste until they able to spit out the toothpaste after every brushing, at this time you may transition to a pea size amount of toothpaste. If your child eats a large amount of toothpaste (you find them with an open tube that appears to be half empty) have them drink milk and contact your dentist, poison control center, or doctor as soon as possible, they may require emergency care. For those children who have a hard time brushing with regular toothpaste we recommend PlaqueHD which has Targetol Techology to help identify and eliminate plaque.
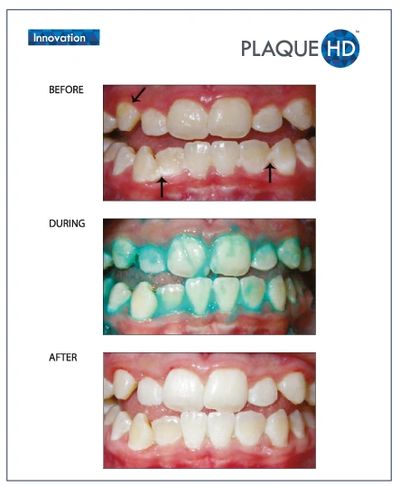
It is very important to maintain the health of the primary teeth. Neglected cavities can and frequently do lead to problems which affect developing permanent teeth.
Primary teeth or baby teeth are important for (1) proper chewing and eating, (2) providing space for the permanent teeth and guiding them into the correct position, and (3) permitting normal development of the jaw bones and muscles.
Primary teeth also affect the development of speech and add to an attractive appearance. While the front 4 teeth last until 6-7 years of age, the back teeth (cuspids and molars) aren’t replaced until age 10-13.
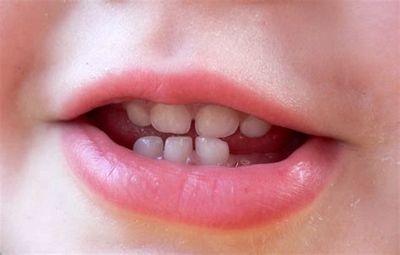
Children’s teeth begin forming before birth. As early as 4 months, the first primary (or baby) teeth to erupt through the gums are the lower central incisors, followed
closely by the upper central incisors.
Although all 20 primary teeth usually appear by age 3, the pace and order of their eruption varies. From the time the first tooth erupts into your child's mouth approximately 4 teeth will erupt every 4 months until all of the baby teeth have
erupted.
Permanent teeth begin appearing around age 6, starting with the first molars and lower central incisors. This process continues until approximately age 21.

Radiographs (X-Rays) are a vital and necessary part of your child’s dental diagnostic process. Without them, certain dental conditions can and will be missed. Radiographs detect much more than cavities. For example, radiographs may be needed to survey erupting teeth, diagnose bone diseases, evaluate the results of an injury, or plan orthodontic treatment.
Radiographs allow dentists to diagnose and treat health conditions that cannot be detected during a clinical examination. If dental problems are found and treated early, dental care is more comfortable for your child and more affordable for you.
The American Academy of Pediatric Dentistry recommends radiographs and examinations every six months for children with a high risk of tooth decay. On average, most pediatric dentists request radiographs approximately once a year. Approximately every 3 years, it is a good idea to obtain a complete set of radiographs, either a panoramic and bitewings or periapicals and bitewings.
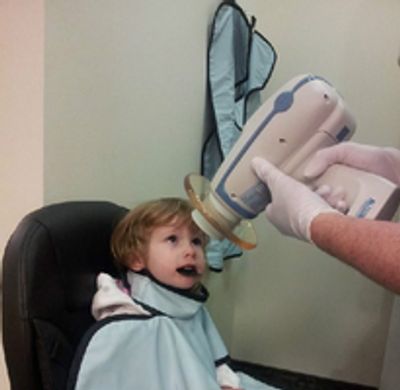
Pediatric dentists are particularly careful to minimize the exposure of their patients to radiation. With contemporary safeguards, the amount of radiation received in a dental X-ray examination is extremely small. The risk is negligible. In fact, the dental radiographs represent a far smaller risk than an undetected and untreated dental problem. Lead body aprons and shields will protect your child. Today’s equipment filters out unnecessary x-rays and restricts the x-ray beam to the area of interest. High-speed film or digital radiographs and proper shielding assure that your child receives a minimal amount of radiation exposure.
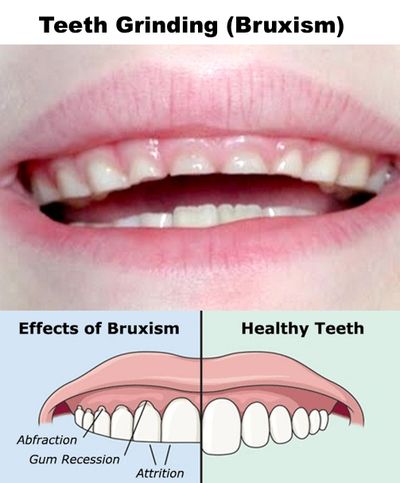
Parents are often concerned about the nocturnal grinding of teeth (bruxism). Often, the first indication is the noise created by the child grinding on their teeth during sleep. Or, the parent may notice wear (teeth getting shorter) to the dentition. One theory as to the cause involves a psychological component. Stress due to a new environment, divorce, changes at school; etc. can influence a child to grind their teeth. Another theory relates to pressure in the inner ear at night. If there are pressure changes (like in an airplane during take-off and landing, when people are chewing gum, etc. to equalize pressure) the child will grind by moving his jaw to relieve this pressure.
The majority of cases of pediatric bruxism do not require any treatment. If excessive wear of the teeth (attrition) is present, then a mouth guard (night guard) may be indicated. The negatives to a mouth guard are the possibility of choking if the appliance becomes dislodged during sleep and it may interfere with growth of the jaws. The positive is obvious by preventing wear to the primary dentition.
The good news is most children outgrow bruxism. The grinding decreases between the ages 6-9 and children tend to stop grinding between ages 9-12. If you suspect bruxism, discuss this with your pediatrician or pediatric dentist.
Sucking is a natural reflex and infants and young children may use thumbs, fingers, pacifiers and other objects on which to suck. It may make them feel secure and happy, or provide a sense of security at difficult periods. Since thumb sucking is relaxing, it may induce sleep.
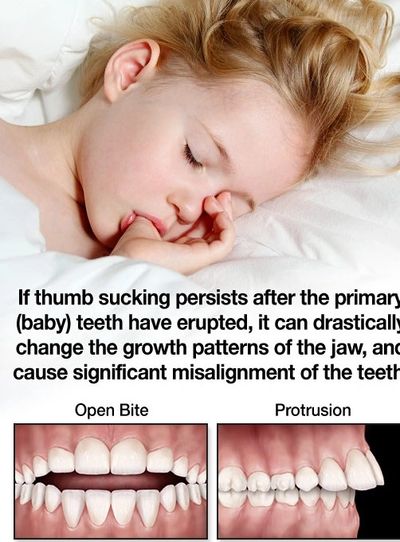
Thumb sucking that persists beyond the eruption of the permanent teeth can cause problems with the proper growth of the mouth and tooth alignment. How intensely and how long a child sucks on fingers or thumbs will determine whether or not dental problems may result. Children who rest their thumbs passively in their mouths are less likely to have difficulty than those who vigorously suck their thumbs.
Children should cease thumb sucking by the time their permanent front teeth are ready to erupt. Usually, children stop between the ages of 2 and 4. If a child stops around the age of 3 any effects from the sucking habit can usually self correct, but if they continue beyond this age the effects are more likely to remain permanent and may require braces to correct. Peer pressure causes many school-aged children to stop.
Pacifiers are no substitute for thumb sucking. They can affect the teeth essentially the same way as sucking fingers and thumbs. However, use of the pacifier can be controlled and modified more easily than the thumb or finger habit. If you have concerns about thumb sucking or use of a pacifier, consult your pediatric dentist.
A few suggestions to help your child get through thumb sucking:
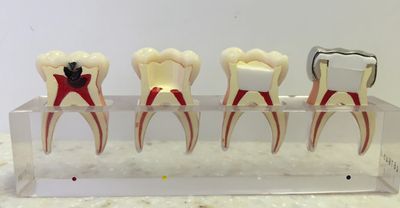
The pulp of a tooth is the inner, central core of the tooth. The pulp contains nerves, blood vessels, connective tissue and reparative cells. The purpose of pulp therapy in Pediatric Dentistry is to maintain the vitality of the affected tooth (so the tooth is not lost).
Dental caries (cavities) and traumatic injury are the main reasons for a tooth to require pulp therapy. Pulp therapy is often referred to as a “nerve treatment”, “children’s root canal”, “pulpectomy” or “pulpotomy”. The two common forms of pulp therapy in children’s teeth are the pulpotomy and pulpectomy.
A pulpotomy removes the diseased pulp tissue within the crown portion of the tooth. Next, an agent is placed to prevent bacterial growth and to calm the remaining nerve tissue. This is followed by a final restoration (usually a stainless steel crown).
A pulpectomy is required when the entire pulp is involved (into the root canal(s) of the tooth). During this treatment, the diseased pulp tissue is completely removed from both the crown and root. The canals are cleansed, disinfected and, in the case of primary teeth, filled with a restorable material. Then, a final restoration is placed. A permanent tooth would be filled with a non-resorbing material.
Developing malocclusions, or bad bites, can be recognized as early as 2-3 years of age. Often, early steps can be taken to reduce the need for major orthodontic treatment at a later age.
Stage I – Early Treatment:
This period of treatment encompasses ages 2 to 6 years. At this young age, we are concerned with underdeveloped dental arches, the premature loss of primary teeth, and harmful habits such as finger or thumb sucking. Treatment initiated in this stage of development is often very successful and many times, though not always, can eliminate the need for future orthodontic/orthopedic treatment.
Stage II – Mixed Dentition:
This period covers the ages of 6 to 12 years, usually beginning with the eruption of the lower permanent incisor (front) teeth and 6 year molars. Many of the malocclusion issues can be addressed at this stage such as crossbites, over or underbites, and crowding. This is an excellent stage to start treatment, when indicated, as your child’s hard and soft tissues are usually very responsive to orthodontic or orthopedic forces and may prevent the necessity of surgery to correct severe malocclusions in the future.
Stage III – Adolescent Dentition:
This stage deals with the permanent teeth and the development of the final bite relationship. This stage is good for finalizing orthodontic treatment, addressing less severe over or underbites, and treating simple crowding cases. Surgery may be required for severe cases if no therapy was provided at a younger age.